Procedures are a tool, not a default
Every procedure on this page has a specific indication — a particular type of pain, confirmed by a particular diagnostic finding, that evidence suggests will respond. Dr. Knopp doesn't offer procedures as a first resort, and he doesn't perform them to fill a schedule. The decision to proceed is always based on whether the intervention is likely to help you, with your specific anatomy and history.
Epidural Steroid Injections (ESI)
An ESI delivers corticosteroid medication directly into the epidural space — the area surrounding the spinal cord and nerve roots. The goal is to reduce inflammation around a compressed or irritated nerve root, not to fix the structural cause. It does not repair a disc or widen a stenotic canal. What it can do is create a window of reduced pain that allows you to participate in rehabilitation and daily activity.
Three approaches — chosen based on your anatomy and pain pattern
- Interlaminar — broad distribution, preferred for cervical levels where precision is critical
- Transforaminal — most targeted; best for unilateral radiculopathy with a single affected nerve root
- Caudal — lower lumbar access; used when anatomy or prior surgery makes other approaches difficult
Who is a candidate?
Radicular pain (pain that travels down an arm or leg) that hasn't resolved after 4–6 weeks of conservative care, with imaging confirming disc herniation or stenosis at the appropriate level, and no signs of progressive neurological deficit. ESI is not appropriate when there is weakness, bladder or bowel changes, or other signs of nerve compromise that require surgical evaluation.
What to expect
The procedure is performed under fluoroscopic (X-ray) guidance with contrast dye to confirm needle placement. Relief typically begins within 3–7 days as the steroid takes effect. Duration varies considerably — from 3 weeks to 12 months, depending on the underlying condition and individual response. A 2025 AAN systematic review (PubMed 39938000) found strong evidence for short-term lumbar radiculopathy relief and moderate evidence for cervical.
Note: cervical transforaminal approaches use only non-particulate steroids (dexamethasone) due to anterior spinal artery anatomy — a safety standard Dr. Knopp follows without exception.
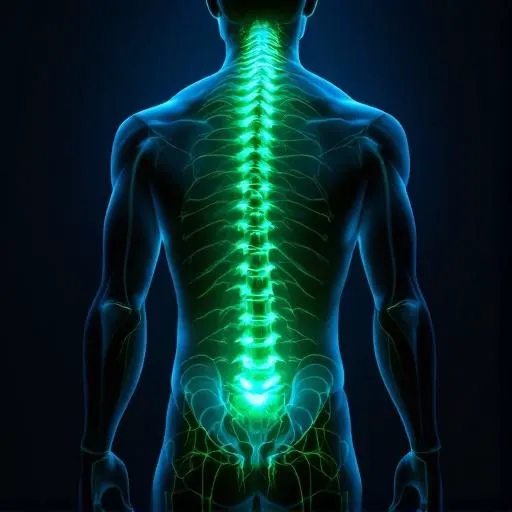
Radiofrequency Ablation (RFA)
RFA uses a probe heated to approximately 80°C to thermally disrupt a specific nerve — the medial branch (for facet joints) or the lateral branch (for the sacroiliac joint). When that nerve can no longer carry pain signals, the joint it was reporting on stops hurting. The nerve eventually regenerates, which is why RFA is not permanent — but the relief it provides is substantially longer than injections alone.
Diagnostic block is required first
RFA is not done on suspicion. A medial branch block (small injection at the nerve, not the joint) must first confirm that the facet joint is actually your pain source. If you achieve ≥80% relief from the diagnostic block, that confirms facet involvement and RFA is indicated. Without this step, the procedure may fail — and Dr. Knopp will not proceed without it.
Who is a candidate?
Confirmed facet joint pain (axial back or neck pain, often worse with extension and rotation, no radiculopathy) or sacroiliac joint pain — both confirmed by diagnostic block. Also used for knee joint denervation in patients who are not candidates for or do not want joint replacement.
Duration and outcomes
Average duration is 6–18 months (approximately 380 days per a 2020 systematic review). The 2025 RAPID trial (PMC12060452) reported that 99.5% of appropriately selected patients achieved ≥50% relief, with 95.8% achieving ≥80% relief. When the nerve regenerates and pain returns, the procedure can be repeated. Cooled RFA is used for sacroiliac joint because the lateral branch anatomy is variable — the larger lesion created by cooled technology improves capture reliability.
Diagnostic & Therapeutic Nerve Blocks
Nerve blocks serve two purposes: they can confirm whether a specific nerve or structure is actually your pain source (diagnostic), and they can provide direct therapeutic relief (therapeutic). In many cases, the same injection does both — which is why they're a valuable tool before committing to longer-term treatment.
Greater Occipital Nerve (GON) Block
For occipital neuralgia, cervicogenic headache, and migraine — injection at the greater occipital nerve at the base of the skull. A 2025 systematic review (PMC11810654, n=562) found 82% of patients achieved ≥30% relief, with 58% achieving ≥50% improvement. Onset is rapid. Can be repeated when relief wears off.
Sacroiliac (SI) Joint Block
Both diagnostic and therapeutic. ≥75% relief from the injection confirms the SI joint as the pain source — which then opens the pathway to lateral branch RFA for longer-lasting relief. Used for posterior pelvic pain, groin referral, and pain that worsens with walking or climbing stairs.
Celiac Plexus Block
For visceral abdominal pain — most commonly from pancreatic cancer or chronic pancreatitis. The celiac plexus is a nerve network in the upper abdomen; blocking it can substantially reduce pain that is otherwise difficult to manage with medications alone.
Peripheral Nerve Stimulation — Sprint PNS
Sprint is a 60-day temporary peripheral nerve stimulation system. A thin wire (lead) is placed percutaneously — through the skin — adjacent to the peripheral nerve responsible for the pain. No incision, no permanent implant. You wear a small external pulse generator for 60 days, then the lead is simply removed.
Relief that outlasts the device
One of the most clinically interesting aspects of Sprint is that sustained relief often continues after the lead is removed. The mechanism is thought to involve central nervous system reconditioning — the nervous system "relearns" a non-pain state during the treatment period. This is not a feature of injections or blocks, which stop working when the medication clears.
Who is a candidate?
Chronic low back pain, shoulder pain, knee pain, peripheral neuropathy, post-surgical pain, and cervicogenic headache are among the conditions with good evidence. Sprint is particularly well-suited for patients who cannot or do not want opioid medications, who have had surgery that hasn't resolved their pain, or who are not candidates for more invasive implantable devices.
Outcomes and access
A real-world outcomes study (N=6,160) found 71% of patients were responders (≥50% pain relief), with an average 63% pain reduction among responders. 75% reduced or eliminated opioid use. Aetna established national coverage effective March 13, 2026, a significant milestone for patient access. ASPN 2025 consensus guidelines confirm Sprint as a safe, cost-effective option before permanent implants.
Dr. Knopp on Sprint: "It's becoming more commonplace, but a lot of doctors and facilities are not doing it — and we're doing it quite a bit."

Spinal Cord Stimulation (SCS)
SCS is a permanently implantable system that delivers electrical pulses to the dorsal epidural space, modulating pain signals before they reach the brain. It is reserved for chronic pain that has not responded adequately to other treatments — and it always begins with a trial before any permanent decision is made.
SCS modalities — technology has advanced significantly
- HF10 (10 kHz, Nevro) — FDA-cleared as superior to traditional SCS. The SENZA RCT showed 80.9% of patients achieved ≥50% back pain relief vs. 42.5% with traditional SCS at 3 months. Paresthesia-free — no tingling sensation.
- Burst SCS — paresthesia-reduced stimulation that targets the affective (emotional) pain pathway, not just the sensory signal. Useful when pain has significant anxiety or suffering components.
- Closed-Loop (EVOKE) — real-time neural signal monitoring with automatic adjustment. Long-term data: 77.6% achieving ≥50% relief at 36 months.
Who is a candidate?
SCS has its strongest evidence for failed back surgery syndrome (Level A), complex regional pain syndrome / CRPS (Level B), and painful peripheral neuropathy. A 7–10 day external trial is always performed first — permanent implantation only proceeds if the trial achieves ≥50% relief. A psychological evaluation is also part of the process, not as a barrier, but as evidence-based patient selection that identifies who will benefit most.
